| Anemia | |
|---|---|
| Other names | Anaemia, erythrocytopenia |
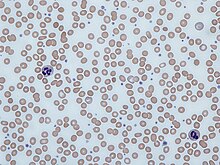 | |
| Blood smear showing iron-deficiency anemia, with small, pale red blood cells | |
| Pronunciation | |
| Specialty | Hematology |
| Symptoms | Feeling tired, pale skin, weakness, shortness of breath, feeling faint[1] |
| Causes | Blood loss, decreased red blood cell production, increased red blood cell breakdown[1] |
| Diagnostic method | Blood hemoglobin measurement[1] |
| Frequency | 1.92 billion / 24% (2021)[2] |
Anemia or anaemia (British English) is a blood disorder in which the blood has a reduced ability to carry oxygen. This can be due to a lower than normal number of red blood cells, a reduction in the amount of hemoglobin available for oxygen transport, or abnormalities in hemoglobin that impair its function.[3][4]
The name is derived from Ancient Greek ἀν- (an-) 'not' and αἷμα (haima) 'blood'.[5] When anemia comes on slowly, the symptoms are often vague, such as tiredness, weakness, shortness of breath, headaches, and a reduced ability to exercise.[1]
When anemia is acute, symptoms may include confusion, feeling like one is going to pass out, loss of consciousness, and increased thirst.[1] Anemia must be significant before a person becomes noticeably pale.[1] Additional symptoms may occur depending on the underlying cause.[1] Anemia can be temporary or long term and can range from mild to severe.[6]
Anemia can be caused by blood loss, decreased red blood cell production, and increased red blood cell breakdown.[1] Causes of blood loss include bleeding due to inflammation of the stomach or intestines, bleeding from surgery, serious injury, or blood donation.[1] Causes of decreased production include iron deficiency, folate deficiency, vitamin B12 deficiency, thalassemia and a number of bone marrow tumors.[1] Causes of increased breakdown include genetic disorders such as sickle cell anemia, infections such as malaria, and certain autoimmune diseases like autoimmune hemolytic anemia.[1]
Anemia can also be classified based on the size of the red blood cells and amount of hemoglobin in each cell.[1] If the cells are small, it is called microcytic anemia; if they are large, it is called macrocytic anemia; and if they are normal sized, it is called normocytic anemia.[1] The diagnosis of anemia in men is based on a hemoglobin of less than 130 to 140 g/L (13 to 14 g/dL); in women, it is less than 120 to 130 g/L (12 to 13 g/dL).[1][7] Further testing is then required to determine the cause.[1][8]
Treatment depends on the specific cause. Certain groups of individuals, such as pregnant women, can benefit from the use of iron pills for prevention.[1][9] Dietary supplementation, without determining the specific cause, is not recommended.[1] The use of blood transfusions is typically based on a person's signs and symptoms.[1] In those without symptoms, they are not recommended unless hemoglobin levels are less than 60 to 80 g/L (6 to 8 g/dL).[1][10] These recommendations may also apply to some people with acute bleeding.[1] Erythropoiesis-stimulating agents are only recommended in those with severe anemia.[10]
Anemia is the most common blood disorder, affecting about a fifth to a third of the global population.[1][11][12][13] Iron-deficiency anemia is the most common cause of anemia worldwide, and affects nearly one billion people.[14]
In 2013, anemia due to iron deficiency resulted in about 183,000 deaths – down from 213,000 deaths in 1990.[15] This condition is most prevalent in children[16][17] with also an above average prevalence in elderly[1] and women of reproductive age (especially during pregnancy).[14] Anemia is one of the six WHO global nutrition targets for 2025 and for diet-related global targets endorsed by World Health Assembly in 2012 and 2013. Efforts to reach global targets contribute to reaching Sustainable Development Goals (SDGs),[18] with anemia as one of the targets in SDG 2 for achieving zero world hunger.[19]
- ^ a b c d e f g h i j k l m n o p q r s t u v Janz TG, Johnson RL, Rubenstein SD (November 2013). "Anemia in the emergency department: evaluation and treatment". Emergency Medicine Practice. 15 (11): 1–15, quiz 15–16. PMID 24716235.
- ^ Gardner WM, et al. (2023). "Prevalence, years lived with disability, and trends in anaemia burden by severity and cause, 1990–2021: findings from the Global Burden of Disease Study 2021". The Lancet Haematology. 10 (9): e713–e734. doi:10.1016/s2352-3026(23)00160-6. hdl:2164/22615. ISSN 2352-3026. PMID 37536353.
- ^ "Anemia: Practice Essentials, Pathophysiology, Etiology". November 9, 2021. Retrieved February 8, 2022.
- ^ "Anemia | NHLBI, NIH". www.nhlbi.nih.gov. Retrieved February 8, 2022.
- ^ "anaemia". Dictionary.com. Archived from the original on July 14, 2014. Retrieved July 7, 2014.
- ^ "Anemia - Symptoms and causes". Mayo Clinic. Retrieved April 1, 2022.
- ^ Smith RE (March 2010). "The clinical and economic burden of anemia". The American Journal of Managed Care. 16 Suppl Issues: S59–66. PMID 20297873.
- ^ Rhodes CE, Denault D, Varacallo M (2024). "Physiology, Oxygen Transport". StatPearls. StatPearls Publishing. PMID 30855920.
- ^ Bhutta ZA, Das JK, Rizvi A, Gaffey MF, Walker N, Horton S, Webb P, Lartey A, Black RE (August 2013). "Evidence-based interventions for improvement of maternal and child nutrition: what can be done and at what cost?". Lancet. 382 (9890): 452–477. doi:10.1016/S0140-6736(13)60996-4. PMID 23746776. S2CID 11748341.
- ^ a b Qaseem A, Humphrey LL, Fitterman N, Starkey M, Shekelle P (December 2013). "Treatment of anemia in patients with heart disease: a clinical practice guideline from the American College of Physicians". Annals of Internal Medicine. 159 (11): 770–779. doi:10.7326/0003-4819-159-11-201312030-00009. PMID 24297193. S2CID 4712203.
- ^ Vos T, et al. (October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ^ Peyrin-Biroulet L, Williet N, Cacoub P (December 1, 2015). "Guidelines on the diagnosis and treatment of iron deficiency across indications: a systematic review". The American Journal of Clinical Nutrition. 102 (6): 1585–1594. doi:10.3945/ajcn.114.103366. PMID 26561626.
- ^ "Anemia Treatment Drugs: 2019 Global Market Study; Analyzed by Type of Anemia, Type of Drug, and Geography". GlobeNewswire (Press release). April 26, 2019. Retrieved August 2, 2023.
- ^ a b Vos T, et al. (December 2012). "Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010". Lancet. 380 (9859): 2163–2196. doi:10.1016/S0140-6736(12)61729-2. PMC 6350784. PMID 23245607.
- ^ GBD 2013 Mortality Causes of Death Collaborators (January 2015). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/S0140-6736(14)61682-2. PMC 4340604. PMID 25530442.
- ^ "WHO Global Anaemia estimates, 2021 Edition". Wolrd Health Organization. Retrieved February 27, 2022.
- ^ Islam MA (December 6, 2021). "Modeling the impact of campaign program on the prevalence of anemia in children under five: Anemia model". Journal of Mathematical Analysis and Modeling. 2 (3): 29–40. doi:10.48185/jmam.v2i3.362. ISSN 2709-5924.
- ^ "WHO | Interventions by global target". www.who.int. World Health Organization. Archived from the original on August 14, 2016.
- ^ "The case for action on anemia". Devex. June 14, 2016.