| Cellulitis | |
|---|---|
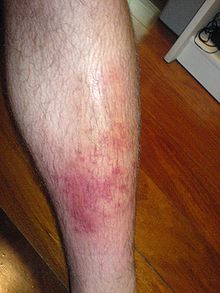 | |
| Skin cellulitis | |
| Specialty | Infectious disease, dermatology |
| Symptoms | Red, hot, painful area of skin, fever[1][2] |
| Duration | 7–10 days[2] |
| Causes | Bacteria[1] |
| Risk factors | Break in the skin, obesity, leg swelling, old age[1] |
| Diagnostic method | Based on symptoms[1][3] |
| Differential diagnosis | Deep vein thrombosis, stasis dermatitis, erysipelas, Lyme disease, necrotizing fasciitis. Sepsis must be ruled out, and if it occurs, must be rapidly treated.[1][4][5] |
| Treatment | Elevation of the affected area[4] |
| Medication | Antibiotics such as cephalexin[1][6] |
| Frequency | 21.2 million (2015)[7] |
| Deaths | 16,900 (2015)[8] |
Cellulitis is usually[9] a bacterial infection involving the inner layers of the skin.[1] It specifically affects the dermis and subcutaneous fat.[1] Signs and symptoms include an area of redness which increases in size over a few days.[1] The borders of the area of redness are generally not sharp and the skin may be swollen.[1] While the redness often turns white when pressure is applied, this is not always the case.[1] The area of infection is usually painful.[1] Lymphatic vessels may occasionally be involved,[1][4] and the person may have a fever and feel tired.[2]
The legs and face are the most common sites involved, although cellulitis can occur on any part of the body.[1] The leg is typically affected following a break in the skin.[1] Other risk factors include obesity, leg swelling, and old age.[1] For facial infections, a break in the skin beforehand is not usually the case.[1] The bacteria most commonly involved are streptococci and Staphylococcus aureus.[1] In contrast to cellulitis, erysipelas is a bacterial infection involving the more superficial layers of the skin, present with an area of redness with well-defined edges, and more often is associated with a fever.[1] The diagnosis is usually based on the presenting signs and symptoms, while a cell culture is rarely possible.[1][3] Before making a diagnosis, more serious infections such as an underlying bone infection or necrotizing fasciitis should be ruled out.[4]
Treatment is typically with antibiotics taken by mouth, such as cephalexin, amoxicillin or cloxacillin.[1][6] Those who are allergic to penicillin may be prescribed erythromycin or clindamycin instead.[6] When methicillin-resistant S. aureus (MRSA) is a concern, doxycycline or trimethoprim/sulfamethoxazole may, in addition, be recommended.[1] There is concern related to the presence of pus or previous MRSA infections.[1][2] Elevating the infected area may be useful, as may pain killers.[4][6]
Potential complications include abscess formation.[1] Around 95% of people are better after 7 to 10 days of treatment.[2] Those with diabetes, however, often have worse outcomes.[10] Cellulitis occurred in about 21.2 million people in 2015.[7] In the United States about 2 of every 1,000 people per year have a case affecting the lower leg.[1] Cellulitis in 2015 resulted in about 16,900 deaths worldwide.[8] In the United Kingdom, cellulitis was the reason for 1.6% of admissions to a hospital.[6]
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y Vary JC, O'Connor, KM (May 2014). "Common Dermatologic Conditions". Medical Clinics of North America. 98 (3): 445–85. doi:10.1016/j.mcna.2014.01.005. PMID 24758956.
- ^ a b c d e Mistry RD (Oct 2013). "Skin and soft tissue infections". Pediatric Clinics of North America. 60 (5): 1063–82. doi:10.1016/j.pcl.2013.06.011. PMID 24093896.
- ^ a b Edwards G, Freeman K, Llewelyn MJ, Hayward G (12 February 2020). "What diagnostic strategies can help differentiate cellulitis from other causes of red legs in primary care?" (PDF). BMJ. 368: m54. doi:10.1136/bmj.m54. PMID 32051117. S2CID 211100166.
- ^ a b c d e Tintinalli, Judith E. (2010). Emergency Medicine: A Comprehensive Study Guide (Emergency Medicine (Tintinalli)) (7th ed.). New York: McGraw-Hill Companies. p. 1016. ISBN 978-0-07-148480-0.
- ^ Wormser GP, Dattwyler RJ, Shapiro ED, Halperin JJ, Steere AC, Klempner MS, Krause PJ, Bakken JS, Strle F, Stanek G, Bockenstedt L, Fish D, Dumler JS, Nadelman RB (1 November 2006). "The Clinical Assessment, Treatment, and Prevention of Lyme Disease, Human Granulocytic Anaplasmosis, and Babesiosis: Clinical Practice Guidelines by the Infectious Diseases Society of America". Clinical Infectious Diseases. 43 (9): 1089–1134. doi:10.1086/508667. PMID 17029130.
- ^ a b c d e Phoenix G, Das, S, Joshi, M (Aug 7, 2012). "Diagnosis and management of cellulitis". BMJ. Clinical Research. 345: e4955. doi:10.1136/bmj.e4955. PMID 22872711. S2CID 28902459.
- ^ a b GBD 2015 Disease and Injury Incidence and Prevalence Collaborators (8 October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ^ a b GBD 2015 Mortality and Causes of Death Collaborators (8 October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/S0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ^ Bansal S, Nimmatoori DP, Singhania N, Lin RC, Nukala CM, Singh AK, Singhania G (3 November 2020). "Severe nonbacterial preseptal cellulitis from adenovirus detected via pooled meta-genomic testing". Clinical Case Reports. 8 (12): 3503–3506. doi:10.1002/ccr3.3468. PMC 7752574. PMID 33363960.
- ^ Dryden M (Sep 2015). "Pathophysiology and burden of infection in patients with diabetes mellitus and peripheral vascular disease: focus on skin and soft-tissue infections". Clinical Microbiology and Infection. 21: S27–S32. doi:10.1016/j.cmi.2015.03.024. PMID 26198368.