| Eosinophil | |
|---|---|
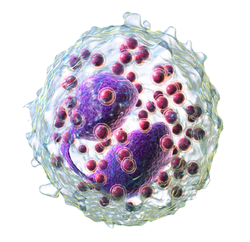 3D rendering of eosinophil | |
 Eosinophil under the microscope (400×) from a peripheral blood smear. Red blood cells surround the eosinophil, two platelets at the top left corner. | |
| Details | |
| Pronunciation | /ˌiːoʊˈsɪnəfɪl/)[1] |
| System | Immune system |
| Identifiers | |
| MeSH | D004804 |
| TH | H2.00.04.1.02017 |
| FMA | 62861 |
| Anatomical terms of microanatomy | |
Eosinophils, sometimes called eosinophiles or, less commonly, acidophils, are a variety of white blood cells and one of the immune system components responsible for combating multicellular parasites and certain infections in vertebrates.[2] Along with mast cells and basophils, they also control mechanisms associated with allergy and asthma. They are granulocytes that develop during hematopoiesis in the bone marrow before migrating into blood, after which they are terminally differentiated and do not multiply.[3]
These cells are eosinophilic or "acid-loving" due to their large acidophilic cytoplasmic granules, which show their affinity for acids by their affinity to coal tar dyes: Normally transparent, it is this affinity that causes them to appear brick-red after staining with eosin, a red dye, using the Romanowsky method.[4] The staining is concentrated in small granules within the cellular cytoplasm, which contain many chemical mediators, such as eosinophil peroxidase, ribonuclease (RNase), deoxyribonucleases (DNase), lipase, plasminogen, and major basic protein. These mediators are released by a process called degranulation following activation of the eosinophil, and are toxic to both parasite and host tissues.
In normal individuals, eosinophils make up about 1–3% of white blood cells, and are about 12–17 micrometres in size with bilobed nuclei.[3][5] While eosinophils are released into the bloodstream, they reside in tissue.[4] They are found in the medulla and the junction between the cortex and medulla of the thymus, and, in the lower gastrointestinal tract, ovaries, uterus, spleen, prostate, and lymph nodes, but not in the lungs, skin, esophagus, or some other internal organs[vague] under normal conditions. The presence of eosinophils in these latter organs is associated with disease. For instance, patients with eosinophilic asthma have high levels of eosinophils that lead to inflammation and tissue damage, making it more difficult for patients to breathe.[6][7] Eosinophils persist in the circulation for 8–12 hours, and can survive in tissue for an additional 8–12 days in the absence of stimulation.[8] Pioneering work in the 1980s elucidated that eosinophils were unique granulocytes, having the capacity to survive for extended periods of time after their maturation as demonstrated by ex-vivo culture experiments.[9]
- ^ "eosinophil - Definition of eosinophil in English by Oxford Dictionaries". Oxford Dictionaries - English. Archived from the original on 8 February 2018. Retrieved 27 March 2018.
- ^ "What is an Eosinophil? | Definition & Function | CCED". www.cincinnatichildrens.org. Retrieved 14 June 2018.
- ^ a b Uhm TG, Kim BS, Chung IY (March 2012). "Eosinophil development, regulation of eosinophil-specific genes, and role of eosinophils in the pathogenesis of asthma". Allergy, Asthma & Immunology Research. 4 (2): 68–79. doi:10.4168/aair.2012.4.2.68. PMC 3283796. PMID 22379601.
- ^ a b Rosenberg HF, Phipps S, Foster PS (June 2007). "Eosinophil trafficking in allergy and asthma". The Journal of Allergy and Clinical Immunology. 119 (6): 1303–10, quiz 1311–2. doi:10.1016/j.jaci.2007.03.048. hdl:1885/30451. PMID 17481712.
- ^ Young B, Lowe jo, Stevens A, Heath JW (2006). Wheater's Functional Histology (5th ed.). Elsevier Limited. ISBN 978-0-443-06850-8.
- ^ Lambrecht BN, Hammad H (January 2015). "The immunology of asthma". Nature Immunology. 16 (1): 45–56. doi:10.1038/ni.3049. PMID 25521684. S2CID 5451867.
- ^ Sanderson, Colin (1992). "Interleukin-5, Eosinophils, and Disease". Blood. 79 (12): 3101–3109. doi:10.1182/blood.V79.12.3101.bloodjournal79123101. PMID 1596561.
- ^ Young B, Lowe JS, Stevens A, Heath JW (2006). Wheater's Functional Histology (5th ed.). Elsevier Limited. ISBN 978-0-443-06850-8.
- ^ Park YM, Bochner BS (April 2010). "Eosinophil survival and apoptosis in health and disease". Allergy, Asthma & Immunology Research. 2 (2): 87–101. doi:10.4168/aair.2010.2.2.87. PMC 2846745. PMID 20358022.