| Mpox | |
|---|---|
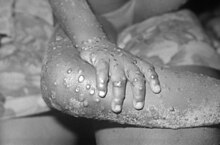 | |
| Mpox rash on arm and leg of a four-year-old girl in 1971 | |
| Pronunciation | |
| Specialty | Infectious disease[1] |
| Symptoms | Rash, fever, exhaustion, swollen lymph nodes, muscle aches, sore throat[2] |
| Complications | Secondary infections, pneumonia, sepsis, encephalitis, and loss of vision with severe eye infection[1] |
| Usual onset | 3–17 days post exposure[2] |
| Duration | 2 to 4 weeks[citation needed] |
| Types | Clade I, Clade II; subclades Ia, Ib, IIa, IIb[3] |
| Causes | Monkeypox virus |
| Diagnostic method | Testing for viral DNA[1] |
| Differential diagnosis | Chickenpox, smallpox[4] |
| Prevention | Smallpox & mpox vaccine, hand washing, covering rash, PPE, social distancing[1] |
| Treatment | Supportive[1] |
| Medication | Tecovirimat, antivirals[1] |
| Prognosis | Most recover[5] |
Mpox (/ˈɛmpɒks/, EM-poks; formerly known as monkeypox)[6] is an infectious viral disease that can occur in humans and other animals. Symptoms include a rash that forms blisters and then crusts over, fever, and swollen lymph nodes. The illness is usually mild, and most infected individuals recover within a few weeks without treatment. The time from exposure to the onset of symptoms ranges from three to seventeen days, and symptoms typically last from two to four weeks. However, cases may be severe, especially in children, pregnant women, or people with suppressed immune systems.[7][8][9]
The disease is caused by the monkeypox virus, a zoonotic virus in the genus Orthopoxvirus. The variola virus, which causes smallpox, is also in this genus.[1] Human-to-human transmission can occur through direct contact with infected skin or body fluids, including sexual contact.[1] People remain infectious from the onset of symptoms until all the lesions have scabbed and healed.[7] The virus may spread from infected animals through handling infected meat or via bites or scratches.[7] Diagnosis can be confirmed by polymerase chain reaction (PCR) testing a lesion for the virus's DNA.[1]
Vaccination is recommended for those at high risk of infection.[1] No vaccine has been developed specifically against mpox, but smallpox vaccines have been found to be effective.[10] There is no specific treatment for the disease, so the aim of treatment is to manage the symptoms and prevent complications.[1][11] Antiviral drugs such as tecovirimat can be used to treat mpox,[1] although their effectiveness has not been proved.[12]
Mpox is endemic in Central and Western Africa, where several species of mammals are suspected to act as a natural reservoir of the virus.[1] The first human cases were diagnosed in 1970 in Basankusu, Democratic Republic of the Congo.[13] Since then, the frequency and severity of outbreaks have significantly increased, possibly as a result of waning immunity since the cessation of routine smallpox vaccination.[13] A global outbreak of clade II in 2022–2023 marked the first incidence of widespread community transmission outside of Africa. In July 2022, the World Health Organization (WHO) declared the outbreak a public health emergency of international concern (PHEIC). The WHO reverted this status in May 2023,[14] as the outbreak came under control, citing a combination of vaccination and public health information as successful control measures.[15]
An outbreak of new variant of clade I mpox (known as clade Ib) was detected in the Democratic Republic of the Congo during 2023.[16] As of August 2024, it had spread to several African countries, raising concerns that it may have adapted to more sustained human transmission.[17][18] In August 2024, the WHO declared the outbreak a public health emergency of international concern.[19][14]
- ^ a b c d e f g h i j k l m "WHO Factsheet – Mpox (Monkeypox)". World Health Organization (WHO). 18 April 2023. Archived from the original on 21 April 2022. Retrieved 21 May 2023.
- ^ a b Cite error: The named reference
CDC_Symwas invoked but never defined (see the help page). - ^ Cite error: The named reference
UKHSAwas invoked but never defined (see the help page). - ^ Cite error: The named reference
Mc2014was invoked but never defined (see the help page). - ^ Cite error: The named reference
Gov.UK2022was invoked but never defined (see the help page). - ^ "WHO recommends new name for monkeypox disease" (Press release). World Health Organization (WHO). 28 November 2022. Archived from the original on 1 December 2022. Retrieved 29 November 2022.
- ^ a b c "Mpox". World Health Organization (WHO). 17 August 2024. Archived from the original on 19 August 2024. Retrieved 22 August 2024.
- ^ "WHO Factsheet – Mpox (Monkeypox)". World Health Organization (WHO). 18 April 2023. Archived from the original on 21 April 2022. Retrieved 21 May 2023.
- ^ "Mpox Symptoms". U.S. Centers for Disease Control and Prevention (CDC). 15 March 2024. Archived from the original on 2 April 2024. Retrieved 22 August 2024.
- ^ Christodoulidou MM, Mabbott NA (1 January 2023). "Efficacy of smallpox vaccines against Mpox infections in humans". Immunotherapy Advances. 3 (1): ltad020. doi:10.1093/immadv/ltad020. PMC 10598838. PMID 37886620.
- ^ "Mpox (formerly Monkeypox)". NIH: National Institute of Allergy and Infectious Diseases. 6 December 2022. Archived from the original on 23 May 2023. Retrieved 24 May 2023.
- ^ "Patient's Guide to Mpox Treatment with Tecovirimat (TPOXX)". U.S. Centers for Disease Control and Prevention (CDC). 28 November 2022. Archived from the original on 24 May 2023. Retrieved 24 May 2023.
- ^ a b Bunge EM, Hoet B, Chen L, Lienert F, Weidenthaler H, Baer LR, et al. (February 2022). "The changing epidemiology of human monkeypox-A potential threat? A systematic review". PLOS Neglected Tropical Diseases. 16 (2): e0010141. doi:10.1371/journal.pntd.0010141. PMC 8870502. PMID 35148313.
- ^ a b "WHO Director-General declares mpox outbreak a public health emergency of international concern". World Health Organization (WHO) (Press release). 14 August 2024. Retrieved 19 October 2024.
- ^ "Mpox (monkeypox) Outbreak". World Health Organization (WHO). Archived from the original on 31 July 2022. Retrieved 13 May 2023.
- ^ "Clade I Mpox Outbreak Originating in Central Africa". U.S. Centers for Disease Control and Prevention (CDC). 10 October 2024. Retrieved 20 October 2024.
- ^ "How scientists are racing to understand the new Mpox strain in the Democratic Republic of the Congo". Gavi, the Vaccine Alliance. 30 July 2024. Retrieved 6 August 2024.
- ^ Cite error: The named reference
:1was invoked but never defined (see the help page). - ^ "WHO declares mpox a public health emergency as newer strain spreads in Africa". MSN. 14 August 2024. Retrieved 14 August 2024.