| Progressive vaccinia | |
|---|---|
| Other names | Vaccinia gangrenosum, Vaccinia necrosum or disseminated vaccinia |
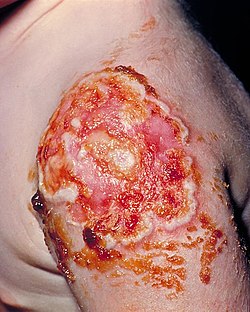 | |
| The patient required a skin graft on her upper left arm in order to correct the necrotic vaccination site, due to the onset of progressive vaccinia, formerly known as vaccinia gangrenosum. | |
| Specialty | Dermatology |
| Symptoms | Malaise, fever, vomiting and tender, enlarged axillary lymph nodes; progresses to septic Pseudomonas aeruginosa, likely from a perirectal abscess, Clostridioides difficile (bacteria), Staphylococcus aureus and cell-mediated immunodeficiency. |
| Complications | Necrosis of the injected part, exacerbating to gangrene and eventual amputation. Usually, the pocks tend to go away without scarring; however, the external and internal spread of the virus may have serious consequences in persons with eczema and other forms of atopic dermatitis, in these persons, defects of innate immunity and a high level of Th2 cell activity render the skin unusually permissive to the initiation and rapid spread of vaccinia infection (known as “eczema vaccinatum”)[1][2] |
| Usual onset | 11 days to 6.5 weeks |
| Duration | Long-lasting |
| Causes | Injection by the vaccinia virus (genus: orthopoxvirus) as a countermeasure for smallpox[3] |
| Risk factors | People with cellular immunodeficiencies |
| Diagnostic method | Fever and headache, then progressive ulceration and necrosis of the injection site for smallpox, albeit the lack of inflammation is noted as the "hallmark of PV"[3] |
| Differential diagnosis | May initially be mistaken for leukemia |
| Prevention | Unknown |
| Treatment | Vaccinia Immune Globulin Intravenous (Human) (VIGIV), Emergency Investigational New Drug (E-IND) both administered orally and topically, (in this case ST-246); CMX001, a lipid conjugate of cidofovir and granulocyte colony-stimulating factor for the exiguous normal white blood cells;supportive care; skin graft |
| Medication | Imiquimod, and thiosemicarbazone |
| Prognosis | Lifelong |
| Frequency | every 1 or 2 in a million during routine vaccination during 1963-1968 for smallpox |
| Deaths | fatality rate: 15% |
Progressive vaccinia is a rare cutaneous condition caused by the vaccinia virus, characterized by painless but progressive necrosis and ulceration.[4]
- ^ Copeman, P. W. M.; Wallace, H. J. (10 October 1964). "Eczema Vaccinatum". BMJ. 2 (5414): 906–908. doi:10.1136/bmj.2.5414.906. PMC 1816899. PMID 14185655.
- ^ Engler, Renata J.M.; Kenner, Julie; Leung, Donald Y.M. (September 2002). Written at Walter Reed Army Medical Center, Allergy-Immunology Department, Washington, DC, USA. "Smallpox vaccination: Risk considerations for patients with atopic dermatitis". Journal of Allergy and Clinical Immunology. 110 (3). Maryland Heights, Missouri, United States: jacionline.org: 357–365. doi:10.1067/mai.2002.128052. PMID 12209080.
- ^ a b Centers for Disease Control Prevention (CDC) (22 May 2009). "Progressive Vaccinia in a Military Smallpox Vaccinee – United States, 2009". Morbidity and Mortality Weekly Report. 58 (19): 532–6. PMID 19478722.
- ^ James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac, eds. (2019). "Progressive Vaccinia (Vaccinia Necrosum, Vaccinia Gangrenosum)". Andrews' Diseases of the Skin E-Book: Clinical Dermatology. Elsevier Health Sciences. p. 388. ISBN 978-0-323-55188-5.