| Sickle cell disease | |
|---|---|
| Other names | Sickle cell disorder; drepanocytosis (dated) |
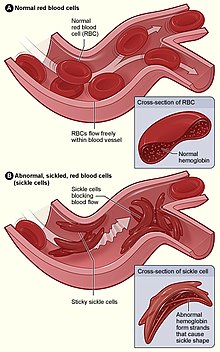 | |
| Figure (A) shows normal red blood cells flowing freely through a blood vessel. The inset shows a cross-section of a normal red blood cell with normal haemoglobin. Figure (B) shows abnormal, sickled red blood cells sticking at the branching point in a blood vessel. The inset image shows a cross-section of a sickle cell with long polymerized sickle haemoglobin (HbS) strands stretching and distorting the cell shape to look like a crescent moon. | |
| Specialty | Hematology, medical genetics |
| Symptoms | Attacks of pain, anemia, swelling in the hands and feet, bacterial infections, stroke[1] |
| Complications | Chronic pain, stroke, aseptic bone necrosis, gallstones, leg ulcers, priapism, pulmonary hypertension, vision problems, kidney problems[2] |
| Usual onset | 5–6 months of age[1] |
| Causes | Genetic, Homozygous mutation in the hemoglobin S gene.[3] |
| Diagnostic method | Blood test[4] |
| Treatment | Vaccination, antibiotics, high fluid intake, folic acid supplementation, pain medication, blood transfusions[5][6] |
| Prognosis | Life expectancy 40–60 years (developed world)[2] |
| Frequency | 7.7 million (2021)[7] |
| Deaths | 34,000 p.a. (a contributory factor to a further 376,000 p.a.)[7] |
Sickle cell disease (SCD), also simply called sickle cell, is a group of hemoglobin-related blood disorders typically inherited.[2] The most common type is known as sickle cell anemia.[2] It results in an abnormality in the oxygen-carrying protein haemoglobin found in red blood cells.[2] This leads to the red blood cells adopting an abnormal sickle-like shape under certain circumstances; with this shape, they are unable to deform as they pass through capillaries, causing blockages.[2] Problems in sickle cell disease typically begin around 5 to 6 months of age.[1] A number of health problems may develop, such as attacks of pain (known as a sickle cell crisis) in joints, anemia, swelling in the hands and feet, bacterial infections, dizziness[8] and stroke.[1] The probability of severe symptoms, including long-term pain, increases with age.[2] Without treatment, people with SCD rarely reach adulthood but with good healthcare, median life expectancy is between 58 and 66 years.[9][10] All the major organs are affected by sickle cell disease. The liver, heart, kidneys, gallbladder, eyes, bones, and joints also can suffer damage from the abnormal functions of the sickle cells, and their inability to flow through the small blood vessels correctly.[11]
Sickle cell disease occurs when a person inherits two abnormal copies of the β-globin gene that makes haemoglobin, one from each parent.[3] Several subtypes exist, depending on the exact mutation in each haemoglobin gene.[2] An attack can be set off by temperature changes, stress, dehydration, and high altitude.[1] A person with a single abnormal copy does not usually have symptoms and is said to have sickle cell trait.[3] Such people are also referred to as carriers.[5] Diagnosis is by a blood test, and some countries test all babies at birth for the disease.[4] Diagnosis is also possible during pregnancy.[4]
The care of people with sickle cell disease may include infection prevention with vaccination and antibiotics, high fluid intake, folic acid supplementation, and pain medication.[5][6] Other measures may include blood transfusion and the medication hydroxycarbamide (hydroxyurea).[6] In 2023, new gene therapies were approved involving the genetic modification and replacement of blood forming stem cells in the bone marrow.[12][13]
As of 2021[update], SCD is estimated to affect about 7.7 million people worldwide, directly causing 34,000 annual deaths and a contributory factor to a further 376,000 deaths.[7] About 80% of sickle cell disease cases are believed to occur in Sub-Saharan Africa.[14] It also occurs to a lesser degree in parts of India, Southern Europe, West Asia, North Africa and among people of African origin (sub-Saharan) living in other parts of the world.[15] The condition was first described in the medical literature by American physician James B. Herrick in 1910.[16][17] In 1949, its genetic transmission was determined by E. A. Beet and J. V. Neel.[17] In 1954, it was established that carriers of the abnormal gene are some degree protected against malaria.[17]
- ^ a b c d e "Sickle Cell Disease - Symptoms". National Heart, Lung, and Blood Institute. 20 August 2024. Retrieved 26 October 2024.
- ^ a b c d e f g h "What Is Sickle Cell Disease?". National Heart, Lung, and Blood Institute. 30 September 2024. Retrieved 26 October 2024.
- ^ a b c "Sickle Cell Disease - Causes and Risk Factors". National Heart, Lung, and Blood Institute. 20 August 2024. Retrieved 26 October 2024.
- ^ a b c "Sickle Cell Disease - Diagnosis". National Heart, Lung, and Blood Institute. 9 September 2024. Retrieved 26 October 2024.
- ^ a b c "Sickle-cell disease and other haemoglobin disorders Fact sheet N°308". January 2011. Archived from the original on 9 March 2016. Retrieved 8 March 2016.
- ^ a b c "Sickle Cell Disease - Treatment". National Heart, Lung, and Blood Institute. 30 September 2024. Retrieved 26 October 2024.
- ^ a b c GBD 2021 Sickle Cell Disease Collaborators (August 2023). "Global, regional, and national prevalence and mortality burden of sickle cell disease, 2000-2021: a systematic analysis from the Global Burden of Disease Study 2021". The Lancet. Haematology. 10 (8): e585–e599. doi:10.1016/S2352-3026(23)00118-7. ISSN 2352-3026. PMC 10390339. PMID 37331373.
{{cite journal}}:|last=has generic name (help)CS1 maint: numeric names: authors list (link) - ^ Nelson MD, Bennett DM, Lehman ME, Okonji AI (5 December 2022). "Dizziness, Falls, and Hearing Loss in Adults Living With Sickle Cell Disease". American Journal of Audiology. 31 (4): 1178–1190. doi:10.1044/2022_AJA-22-00059. ISSN 1558-9137. PMID 36251873.
- ^ "Sickle Cell Anemia: Symptoms, What It Is, Causes & Treatment". Cleveland Clinic. Retrieved 8 May 2024.
- ^ "Sickle cell disease: What is the prognosis?". National Institute for Health and Care Excellence. July 2021. Retrieved 25 October 2024.
- ^ "Sickle Cell Disease - How Sickle Cell Disease May Affect Your Health". www.nhlbi.nih.gov. National Heart, Lung, and Blood Institute. 23 April 2024. Retrieved 25 July 2024.
- ^ Cite error: The named reference
FDA PR 20231208was invoked but never defined (see the help page). - ^ Cite error: The named reference
Wilkwas invoked but never defined (see the help page). - ^ Cite error: The named reference
:4was invoked but never defined (see the help page). - ^ Elzouki AY (2012). Textbook of clinical pediatrics (2 ed.). Berlin: Springer. p. 2950. ISBN 9783642022012.
- ^ Savitt TL, Goldberg MF (January 1989). "Herrick's 1910 case report of sickle cell anemia. The rest of the story". The Journal of the American Medical Association. 261 (2): 266–271. doi:10.1001/jama.261.2.266. PMID 2642320.
- ^ a b c Serjeant GR (December 2010). "One hundred years of sickle cell disease". British Journal of Haematology. 151 (5): 425–429. doi:10.1111/j.1365-2141.2010.08419.x. PMID 20955412.