| Basal-cell carcinoma | |
|---|---|
| Other names | Basal-cell skin cancer, basalioma, rodent ulcer |
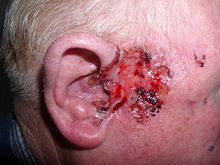 | |
| An ulcerated basal cell carcinoma near the ear of a 75-year-old male | |
| Specialty | Dermatology, oncology |
| Symptoms | Painless raised area of skin that may be shiny with small blood vessel running over it or ulceration[1] |
| Risk factors | Light skin, ultraviolet light, radiation therapy, arsenic, poor immune function[2] |
| Diagnostic method | Examination, skin biopsy[3] |
| Differential diagnosis | Milia, seborrheic keratosis, melanoma, psoriasis[4] |
| Treatment | Surgical removal[2] |
| Prognosis | Good[5] |
| Frequency | ~30% of white people at some point (US)[2] |
| Deaths | Rare[6] |
Basal-cell carcinoma (BCC), also known as basal-cell cancer, basalioma[7] or rodent ulcer,[8] is the most common type of skin cancer.[2] It often appears as a painless raised area of skin, which may be shiny with small blood vessels running over it.[1] It may also present as a raised area with ulceration.[1] Basal-cell cancer grows slowly and can damage the tissue around it, but it is unlikely to spread to distant areas or result in death.[9]
Risk factors include exposure to ultraviolet light, having lighter skin, radiation therapy, long-term exposure to arsenic and poor immune-system function.[2] Exposure to UV light during childhood is particularly harmful.[5] Tanning beds have become another common source of ultraviolet radiation.[10] Diagnosis often depends on skin examination, confirmed by tissue biopsy.[2][3]
It remains unclear whether sunscreen affects the risk of basal-cell cancer.[11] Treatment is typically by surgical removal.[2] This can be by simple excision if the cancer is small; otherwise, Mohs surgery is generally recommended.[2] Other options include electrodesiccation and curettage, cryosurgery, topical chemotherapy, photodynamic therapy, laser surgery or the use of imiquimod, a topical immune-activating medication.[12] In the rare cases in which distant spread has occurred, chemotherapy or targeted therapy may be used.[12]
Basal-cell cancer accounts for at least 32% of all cancers globally.[9][13] Of skin cancers other than melanoma, about 80% are basal-cell cancers.[2] In the United States, about 35% of white males and 25% of white females are affected by BCC at some point in their lives.[2]
Basal-cell carcinoma is named after the basal cells that form the lowest layer of the epidermis. It is thought to develop from the folliculo–sebaceous–apocrine germinative cells called trichoblasts (of note, trichoblastic carcinoma is a term sometimes used to refer to a rare type of aggressive skin cancer that may resemble a benign trichoblastoma, and can also closely resemble basal cell carcinoma).
- ^ a b c "Skin Cancer Treatment (PDQ®)". NCI. 2013-10-25. Archived from the original on 5 July 2014. Retrieved 30 June 2014.
- ^ a b c d e f g h i j Gandhi SA, Kampp J (November 2015). "Skin Cancer Epidemiology, Detection, and Management". The Medical Clinics of North America. 99 (6): 1323–35. doi:10.1016/j.mcna.2015.06.002. PMID 26476255.
- ^ a b "Skin Cancer Treatment". National Cancer Institute. 21 June 2017. Archived from the original on 4 July 2017. Retrieved 2 July 2017.
- ^ Krutmann J, Humbert P (2010). Nutrition for Healthy Skin: Strategies for Clinical and Cosmetic Practice. Springer. p. 31. ISBN 978-3-642-12264-4. Archived from the original on 2017-09-10.
- ^ a b World Cancer Report 2014. World Health Organization. 2014. Chapter 5.14. ISBN 978-92-832-0429-9.
- ^ GBD 2015 Mortality and Causes of Death Collaborators (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ^ "Basal Cell Carcinoma". dermnetnz.org. 26 October 2023. Retrieved 12 November 2023.
- ^ "Basal Cell Carcinoma (Rodent Ulcer or BCC)". Newcastle Hospitals NHS Foundation Trust. 31 October 2022. Retrieved 12 November 2023.
- ^ a b Cakir BÖ, Adamson P, Cingi C (November 2012). "Epidemiology and economic burden of nonmelanoma skin cancer". Facial Plastic Surgery Clinics of North America. 20 (4): 419–22. doi:10.1016/j.fsc.2012.07.004. PMID 23084294.
- ^ Gallagher RP, Lee TK, Bajdik CD, Borugian M (2010). "Ultraviolet radiation". Chronic Diseases in Canada. 29 (Suppl 1): 51–68. doi:10.24095/hpcdp.29.S1.04. PMID 21199599.
The major source of ultraviolet radiation is solar radiation or sunlight. However, exposure to artificial sources particularly through tanning salons is becoming more important in terms of human health effects, as use of these facilities by young people, [sic] has increased.
- ^ Jou PC, Feldman RJ, Tomecki KJ (June 2012). "UV protection and sunscreens: what to tell patients". Cleveland Clinic Journal of Medicine. 79 (6): 427–36. doi:10.3949/ccjm.79a.11110. PMID 22660875. S2CID 44457153.
- ^ a b "Skin Cancer Treatment". National Cancer Institute. 21 June 2017. Archived from the original on 4 July 2017. Retrieved 2 July 2017.
- ^ Dubas LE, Ingraffea A (February 2013). "Nonmelanoma skin cancer". Facial Plastic Surgery Clinics of North America. 21 (1): 43–53. doi:10.1016/j.fsc.2012.10.003. PMID 23369588.