| Extrahepatic biliary atresia | |
|---|---|
| Other names | Extrahepatic ductopenia |
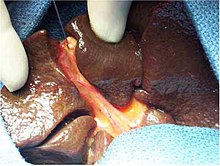 | |
| Intraoperative view of complete extrahepatic biliary atresia[1] | |
| Specialty | Pediatric surgery |
| Symptoms | Jaundice, pale stool, dark urine |
| Complications | Cirrhosis, portal hypertension, liver failure |
| Usual onset | Infancy |
| Types | Congenital, acquired |
| Treatment | Surgery, liver transplantation |
| Frequency | 1 in 5,000 (East Asia), 1 in 10,000-15,000 (US) |
Biliary atresia, also known as extrahepatic ductopenia and progressive obliterative cholangiopathy, is a childhood disease of the liver in which one or more bile ducts are abnormally narrow, blocked, or absent. It can be congenital or acquired. It has an incidence of one in 10,000–15,000 live births in the United States,[2] and a prevalence of one in 16,700 in the British Isles.[3][4] Biliary atresia is most common in East Asia, with a frequency of one in 5,000.
The cause of biliary atresia in Egyptian infants has been proven to be as a result of aflatoxin induced cholangiopathy acquired prenatally in infants who have glutathione S transferase M1 deficiency. The biliary atresia phenotype caused by congenital aflatoxicosis in GST M1 deficient neonates is named Kotb disease.[5] Syndromic biliary atresia (e.g. Biliary Atresia Splenic Malformation (BASM)) has been associated with certain genes (e.g. Polycystic Kidney Disease 1 Like 1 - PKD1L1[6]), and some infants with isolated biliary atresia may arise as a result of an autoimmune inflammatory response, possibly due to a viral infection of the liver soon after birth.[7] In animals plant toxins have been shown to cause biliary atresia.[8] The only effective treatments[9] are operations such as the Kasai procedure and liver transplantation.[10]
- ^ Chardot, Christophe (2006). "Biliary atresia". Orphanet Journal of Rare Diseases. 1: 28. doi:10.1186/1750-1172-1-28. PMC 1560371. PMID 16872500.
- ^ Suchy, Frederick J. (2015). "Anatomy, Histology, Embryology, Developmental Anomalies, and Pediatric Disorders of the Biliary Tract". In Feldman, Mark; Friedman, Lawrence S.; Brandt, Lawrence J. (eds.). Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology, Diagnosis, Management (10th ed.). Elsevier Health Sciences. pp. 1055–77. ISBN 978-1-4557-4989-8.
- ^ McKiernan, Patrick J; Baker, Alastair J; Kelly, Deirdre A (2000). "The frequency and outcome of biliary atresia in the UK and Ireland". The Lancet. 355 (9197): 25–9. doi:10.1016/S0140-6736(99)03492-3. PMID 10615887. S2CID 25981400.
- ^ Hartley, Jane L; Davenport, Mark; Kelly, Deirdre A (2009). "Biliary atresia". The Lancet. 374 (9702): 1704–13. doi:10.1016/S0140-6736(09)60946-6. PMID 19914515. S2CID 24191796.
- ^ Kotb, Magd A.; Kotb, Ahmed (March 2015). "Extrahepatic Biliary Atresia is an Aflatoxin Induced Cholangiopathy in Infants with Null GSTM1 Genotype with Disrupted P53 and GSTPi to Mothers Heterozygous for GSTM1 Polymorphism: Damage Control is Mediated through Neutrophil Elastase and CD14+ Activated Monocytes: Kotb Disease" (PDF). The Medical Journal of Cairo University. 83 (2): 137–145.
- ^ Berauer, John‐Paul; Mezina, Anya I.; Okou, David T.; Sabo, Aniko; Muzny, Donna M.; Gibbs, Richard A.; Hegde, Madhuri R.; Chopra, Pankaj; Cutler, David J.; Perlmutter, David H.; Bull, Laura N.; Thompson, Richard J.; Loomes, Kathleen M.; Spinner, Nancy B.; Rajagopalan, Ramakrishnan; Guthery, Stephen L.; Moore, Barry; Yandell, Mark; Harpavat, Sanjiv; Magee, John C.; Kamath, Binita M.; Molleston, Jean P.; Bezerra, Jorge A.; Murray, Karen F.; Alonso, Estella M.; Rosenthal, Philip; Squires, Robert H.; Wang, Kasper S.; Finegold, Milton J.; Russo, Pierre; Sherker, Averell H.; Sokol, Ronald J.; Karpen, Saul J. (September 2019). "Identification of Polycystic Kidney Disease 1 Like 1 Gene Variants in Children With Biliary Atresia Splenic Malformation Syndrome". Hepatology. 70 (3): 899–910. doi:10.1002/hep.30515. PMC 6642859. PMID 30664273.
- ^ Mack, Cara (2007). "The Pathogenesis of Biliary Atresia: Evidence for a Virus-Induced Autoimmune Disease". Seminars in Liver Disease. 27 (3): 233–42. doi:10.1055/s-2007-985068. PMC 3796656. PMID 17682970.
- ^ Koo, Kyung A.; Lorent, Kristin; Gong, Weilong; Windsor, Peter; Whittaker, Stephen J.; Pack, Michael; Wells, Rebecca G.; Porter, John R. (17 August 2015). "Biliatresone, a Reactive Natural Toxin from Dysphania glomulifera and D. littoralis: Discovery of the Toxic Moiety 1,2-Diaryl-2-Propenone". Chemical Research in Toxicology. 28 (8): 1519–1521. doi:10.1021/acs.chemrestox.5b00227. PMC 4755499. PMID 26175131.
- ^ Superina, Riccardo (December 2017). "Biliary atresia and liver transplantation: results and thoughts for primary liver transplantation in select patients". Pediatric Surgery International. 33 (12): 1297–1304. doi:10.1007/s00383-017-4174-4. PMID 29030698. S2CID 23189323.
- ^ Lien, Tien-Hau; Chang, Mei-Hwei; Wu, Jia-Feng; Chen, Huey-Ling; Lee, Hung-Chang; Chen, An-Chyi; Tiao, Mao-Meng; Wu, Tzee-Chung; Yang, Yao-Jong; Lin, Chieh-Chung; Lai, Ming-Wei; Hsu, Hong-Yuan; Ni, Yen-Hsuan (2011). "Effects of the infant stool color card screening program on 5-year outcome of biliary atresia in Taiwan". Hepatology. 53 (1): 202–8. doi:10.1002/hep.24023. PMID 21140377. S2CID 13397641.