| Catatonia | |
|---|---|
| Other names | Catatonic syndrome |
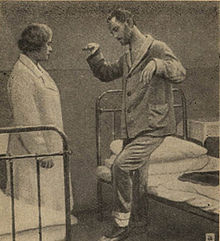 | |
| A patient in catatonic stupor | |
| Specialty | Psychiatry, neurology |
| Symptoms | Immobility, mutism, staring, posturing, rigidity, low consciousness, etc. |
| Complications | Physical trauma, malignant catatonia (autonomic instability, life-threatening), dehydration, pneumonia, pressure ulcers due to immobility, muscle contractions, deep vein thrombosis (DVT)[1] and pulmonary embolism (PE)[1] |
| Causes | Underlying illness (psychiatric, neurologic, or medical), brain injury/damage, certain drugs/medications |
| Diagnostic method | Clinical, lorazepam challenge |
| Treatment | Benzodiazepines (lorazepam challenge), electroconvulsive therapy (ECT)[1] |
Catatonia is a complex syndrome, most commonly seen in people with underlying mood (e.g major depressive disorder) or psychotic disorders (e.g schizophrenia).[2][3] People with catatonia have abnormal movement and behaviors, which vary from person to person and fluctuate in intensity within a single episode.[4] People with catatonia appear withdrawn, meaning that they do not interact with the outside world and have difficulty processing information.[5] They may be nearly motionless for days on end or perform repetitive purposeless movements. Two people may exhibit very different sets of behaviors and both still be diagnosed with catatonia. Treatment with benzodiazepines or ECT are most effective and lead to remission of symptoms in most cases.[3]
There are different subtypes of catatonia, which represent groups of symptoms that commonly occur together. These include stuporous/akinetic catatonia, excited catatonia, malignant catatonia, and periodic catatonia.[6]
Catatonia has historically been related to schizophrenia (catatonic schizophrenia), but is most often seen in mood disorders.[3] It is now known that catatonic symptoms are nonspecific and may be observed in other mental, neurological, and medical conditions.
- ^ a b c Balaguer AP, Rivero IS (22 December 2021). "Electroconvulsive therapy, catatonia, deep vein thrombosis and anticoagulant treatment: a case report". General Psychiatry. 34 (6): e100666. doi:10.1136/gpsych-2021-100666. ISSN 2517-729X. PMC 8705197. PMID 35028525.
- ^ Fink M, Taylor MA (1 November 2009). "The Catatonia Syndrome: Forgotten but Not Gone". Archives of General Psychiatry. 66 (11): 1173–1177. doi:10.1001/archgenpsychiatry.2009.141. PMID 19884605.
- ^ a b c Burrow JP, Spurling BC, Marwaha R (2022). "Catatonia". StatPearls. StatPearls Publishing. PMID 28613592.
- ^ Cite error: The named reference
Heckers 2023was invoked but never defined (see the help page). - ^ Edinoff AN, Kaufman SE, Hollier JW, Virgen CG, Karam CA, Malone GW, Cornett EM, Kaye AM, Kaye AD (8 November 2021). "Catatonia: Clinical Overview of the Diagnosis, Treatment, and Clinical Challenges". Neurology International. 13 (4): 570–586. doi:10.3390/neurolint13040057. ISSN 2035-8385. PMC 8628989. PMID 34842777.
- ^ "UpToDate". www.uptodate.com. Retrieved 22 November 2024.