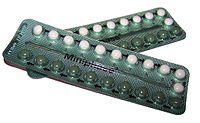
| Combined oral contraceptive pill | |
|---|---|
 | |
| Background | |
| Type | Hormonal |
| First use | 1960 (United States) |
| Failure rates (first year) | |
| Perfect use | 0.3%[1] |
| Typical use | 9%[1] |
| Usage | |
| Duration effect | 1–4 days |
| Reversibility | Yes |
| User reminders | Taken within same 24-hour window each day |
| Clinic review | 6 months |
| Advantages and disadvantages | |
| STI protection | No |
| Periods | Regulated, and often lighter and less painful |
| Weight | No proven effect |
| Benefits | Evidence for reduced mortality risk and reduced death rates in all cancers.[2] Possible reduced ovarian and endometrial cancer risks.[3][citation needed] May treat acne, PCOS, PMDD, endometriosis[citation needed] |
| Risks | Possible small increase in some cancers.[4][5] Small reversible increase in DVTs; stroke,[6] cardiovascular disease[7] |
| Medical notes | |
| Affected by the antibiotic rifampicin,[8] the herb Hypericum (St. Johns Wort) and some anti-epileptics, also vomiting or diarrhea. Caution if history of migraines. | |
The combined oral contraceptive pill (COCP), often referred to as the birth control pill or colloquially as "the pill", is a type of birth control that is designed to be taken orally by women. It is the oral form of combined hormonal contraception. The pill contains two important hormones: a progestin (a synthetic form of the hormone progestogen/progesterone) and estrogen (usually ethinylestradiol or 17β estradiol).[9][10][11][12] When taken correctly, it alters the menstrual cycle to eliminate ovulation and prevent pregnancy.
COCPs were first approved for contraceptive use in the United States in 1960, and remain a very popular form of birth control. They are used by more than 100 million women worldwide [13][14] including about 9 million women in the United States.[15][16] From 2015 to 2017, 12.6% of women aged 15–49 in the US reported using COCPs, making it the second most common method of contraception in this age range (female sterilization is the most common method).[17] Use of COCPs, however, varies widely by country,[18] age, education, and marital status. For example, one third of women aged 16–49 in the United Kingdom use either the combined pill or progestogen-only pill (POP),[19][20] compared with less than 3% of women in Japan (as of 1950–2014).[21]
Combined oral contraceptives are on the World Health Organization's List of Essential Medicines.[22] The pill was a catalyst for the sexual revolution.[23]
- ^ a b Trussell J (2011). "Contraceptive efficacy". In Hatcher RA, Trussell J, Nelson A, Cates W, Kowal D, Policar M (eds.). Contraceptive technology (20th revised ed.). New York: Ardent Media. pp. 779–863. ISBN 978-1-59708-004-0. ISSN 0091-9721. OCLC 781956734. Table 26–1 = Table 3–2 Percentage of women experiencing an unintended pregnancy during the first year of typical use and the first year of perfect use of contraception, and the percentage continuing use at the end of the first year. United States. Archived 15 February 2017 at the Wayback Machine
- ^ Cite error: The named reference
Hannaford 2010was invoked but never defined (see the help page). - ^ "Oral Contraceptives and Cancer Risk". National Cancer Institute. 22 February 2018. Archived from the original on 27 May 2020. Retrieved 10 May 2020.
- ^ Cite error: The named reference
IARC2007was invoked but never defined (see the help page). - ^ Collaborative Group on Hormonal Factors in Breast Cancer (June 1996). "Breast cancer and hormonal contraceptives: collaborative reanalysis of individual data on 53 297 women with breast cancer and 100 239 women without breast cancer from 54 epidemiological studies". Lancet. 347 (9017): 1713–27. doi:10.1016/S0140-6736(96)90806-5. PMID 8656904. S2CID 36136756.
- ^ Kemmeren JM, Tanis BC, van den Bosch MA, Bollen EL, Helmerhorst FM, van der Graaf Y, et al. (May 2002). "Risk of Arterial Thrombosis in Relation to Oral Contraceptives (RATIO) study: oral contraceptives and the risk of ischemic stroke". Stroke. 33 (5): 1202–8. doi:10.1161/01.STR.0000015345.61324.3F. PMID 11988591.
- ^ Baillargeon JP, McClish DK, Essah PA, Nestler JE (July 2005). "Association between the current use of low-dose oral contraceptives and cardiovascular arterial disease: a meta-analysis". The Journal of Clinical Endocrinology and Metabolism. 90 (7): 3863–70. doi:10.1210/jc.2004-1958. PMID 15814774.
- ^ "Birth Control Pills - Birth Control Pill - The Pill". Archived from the original on 5 August 2011. Retrieved 3 April 2009.
- ^ Cite error: The named reference
:02was invoked but never defined (see the help page). - ^ "Guinea pigs or pioneers? How Puerto Rican women were used to test the birth control pill". The Washington Post. ISSN 0190-8286. Archived from the original on 8 November 2022. Retrieved 14 September 2022.
- ^ "Birth Control Pill (for Teens) - Nemours KidsHealth". kidshealth.org. Archived from the original on 21 September 2022. Retrieved 21 September 2022.
- ^ Tyrer L (1999). "Introduction of the pill and its impact". Contraception. 59 (1): 11S–16S. doi:10.1016/s0010-7824(98)00131-0. PMID 10342090.
- ^ Contraceptive use by method 2019 : data booklet. [New York, NY]: United Nations. Department of Economic and Social Affairs. Population Division. 2019. ISBN 978-92-1-148329-1. OCLC 1135665739.
- ^ Christin-Maitre S (February 2013). "History of oral contraceptive drugs and their use worldwide". Best Practice & Research. Clinical Endocrinology & Metabolism. 27 (1): 3–12. doi:10.1016/j.beem.2012.11.004. PMID 23384741.
- ^ "Products - Data Briefs - Number 327 - December 2018". U.S. Centers for Disease Control and Prevention (CDC). 11 July 2022. Archived from the original on 13 September 2022. Retrieved 14 September 2022.
- ^ Sech LA, Mishell DR (November 2015). "Oral steroid contraception". Women's Health. 11 (6): 743–748. doi:10.2217/whe.15.82. PMID 26673988. S2CID 6433771.
- ^ "Current Contraceptive Status Among Women Aged 15–49: United States, 2015–2017". U.S. Centers for Disease Control and Prevention (CDC). 7 June 2019. Archived from the original on 13 September 2022. Retrieved 2 August 2019.
- ^ UN Population Division (2006). World Contraceptive Use 2005 (PDF). New York: United Nations. ISBN 978-92-1-151418-6. Archived (PDF) from the original on 26 April 2018. Retrieved 28 June 2017. women aged 15–49 married or in consensual union
- ^ Delvin D (15 June 2016). "Contraception – the contraceptive pill: How many women take it in the UK?". Archived from the original on 4 January 2011. Retrieved 25 December 2010.
- ^ Taylor T, Keyse L, Bryant A (2006). Contraception and Sexual Health, 2005/06 (PDF). London: Office for National Statistics. ISBN 978-1-85774-638-9. Archived from the original (PDF) on 9 January 2007. British women aged 16–49: 24% use the pill as of 2016[update] (17% use Combined pill, 5% use Minipill, 2% don't know type)
- ^ Yoshida H, Sakamoto H, Leslie A, Takahashi O, Tsuboi S, Kitamura K (June 2016). "Contraception in Japan: Current trends". Contraception. 93 (6): 475–477. doi:10.1016/j.contraception.2016.02.006. PMID 26872717.
- ^ World Health Organization (2023). The selection and use of essential medicines 2023: web annex A: World Health Organization model list of essential medicines: 23rd list (2023). Geneva: World Health Organization. hdl:10665/371090. WHO/MHP/HPS/EML/2023.02.
- ^ Harris G (3 May 2010). "The Pill Started More Than One Revolution". The New York Times. Archived from the original on 27 September 2015. Retrieved 21 September 2015.