| Complex regional pain syndrome | |
|---|---|
| Other names | Algodystrophy; Amplified musculoskeletal pain syndrome; hyponym: reflex sympathetic dystrophy (RSD); hyponym: causalgia; hyponym: reflex neurovascular dystrophy (RND) |
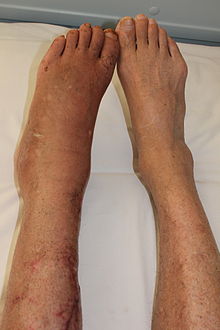 | |
| Leg of an individual (left) with complex regional pain syndrome following tibial bone fracture | |
| Specialty | Neurology, psychiatry, anesthesiology |
| Symptoms | Pain, allodynia, hypo- or hyperesthesia, skin temperature abnormalities, atrophy, stiffness |
| Treatment | Physical therapy (more effective with early diagnosis); medications (e.g., anticonvulsants, opioids, muscle relaxers, etc.); sympathetic nerve blockade; ketamine infusions; lidocaine infusions; implantable pharmaceuticals; amputation |
| Medication | Anticonvulsants (e.g., gabapentin); muscle relaxers (e.g., baclofen), ketamine or lidocaine infusions[citation needed] |
Complex regional pain syndrome (CRPS Type 1 and Type 2) is a severe form of chronic pain, in which pain from a physical trauma outlasts the expected recovery time. The symptoms of types 1 and 2 are the same except type 2 is associated with nerve injury.
Usually starting in a limb, CRPS manifests as pain, swelling, limited range of motion, and/or changes to the skin and bones. It may initially affect one limb and then spread throughout the body; 35% of affected individuals report symptoms throughout the body.[1] Two types are thought to exist: CRPS type 1 (previously referred to as reflex sympathetic dystrophy) and CRPS type 2 (previously referred to as causalgia). It is possible to have both types.[2]
Amplified musculoskeletal pain syndrome, a condition that is similar to CRPS, primarily affects pediatric patients, falls under rheumatology and pediatrics, and is generally considered a subset of CRPS type I.[3]
- ^ Schwartzman, R.J.; Erwin, K.L.; Alexander, G.M. (May 2009). "The natural history of complex regional pain syndrome". The Clinical Journal of Pain. 25 (4): 273–280. doi:10.1097/AJP.0b013e31818ecea5. PMID 19590474. S2CID 10909080.
- ^ Harden, R.N.; Bruehl, S.; Stanton-Hicks, M.; Wilson, P.R. (May 2007). "Proposed new diagnostic criteria for complex regional pain syndrome". Pain Medicine. 8 (4): 326–331. doi:10.1111/j.1526-4637.2006.00169.x. PMID 17610454.
- ^ "Amplified Musculoskeletal Pain Syndrome (AMPS) in Children". Cleveland Clinic. Retrieved 2024-02-10.