| Congenital syphilis | |
|---|---|
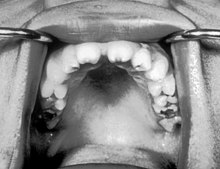 | |
| Notched incisors known as Hutchinson's teeth which are characteristic of congenital syphilis | |
| Specialty | Infectious diseases |
| Symptoms | Rash, fever, large liver and spleen, skeletal abnormalities[1] |
| Usual onset | Unborn baby, newborn baby or later[1] |
| Duration | Lifelong |
| Types | Early & late[2] |
| Causes | Treponema pallidum[2] |
| Diagnostic method | Signs, symptoms, blood tests, CSF tests |
| Prevention | Adequate screening and treatment in pregnant mother[2] |
| Treatment | Antibiotic[3] |
| Medication | Penicillin by injection; Procaine benzylpenicillin, benzylpenicillin, benzathine penicillin G[3] |

Congenital syphilis is syphilis that occurs when a mother with untreated syphilis passes the infection to her baby during pregnancy or at birth.[4] It may present in the fetus, infant, or later.[1][5] Clinical features vary and differ between early onset, that is presentation before 2-years of age, and late onset, presentation after age 2-years.[4] Infection in the unborn baby may present as poor growth, non-immune hydrops leading to premature birth or loss of the baby, or no signs.[2][4] Affected newborns mostly initially have no clinical signs.[4] They may be small and irritable.[4] Characteristic features include a rash, fever, large liver and spleen, a runny and congested nose, and inflammation around bone or cartilage.[2][4] There may be jaundice, large glands, pneumonia (pneumonia alba), meningitis, warty bumps on genitals, deafness or blindness.[4][6][7] Untreated babies that survive the early phase may develop skeletal deformities including deformity of the nose, lower legs, forehead, collar bone, jaw, and cheek bone.[4] There may be a perforated or high arched palate, and recurrent joint disease.[2][4] Other late signs include linear perioral tears, intellectual disability, hydrocephalus, and juvenile general paresis.[4] Seizures and cranial nerve palsies may first occur in both early and late phases.[4] Eighth nerve palsy, interstitial keratitis and small notched teeth may appear individually or together; known as Hutchinson's triad.[4]
It is caused by the bacterium Treponema pallidum subspecies pallidum when it infects the baby after crossing the placenta or from contact with a syphilitic sore at birth.[4][5] It is not transmitted during breastfeeding unless there is an open sore on the mother's breast.[4] The unborn baby can become infected at any time during the pregnancy.[4] Most cases occur due to inadequate antenatal screening and treatment during pregnancy.[8] The baby is highly infectious if the rash and snuffles are present.[4] The disease may be suspected from tests on the mother; blood tests and ultrasound.[9] Tests on the baby may include blood tests, CSF analysis and medical imaging.[10] Findings may reveal anemia and low platelets.[4] Other findings may include low sugars, proteinuria and hypopituitarism.[4] The placenta may appear large and pale.[4] Other investigations include testing for HIV.[10]
Prevention is by safe sex to prevent syphilis in the mother, and early screening and treatment of syphilis in pregnancy.[6] One intramuscular injection of benzathine penicillin G administered to a pregnant woman early in the illness can prevent congenital syphilis in her baby.[11] Treatment of suspected congenital syphilis is with penicillin by injection; benzylpenicillin into vein, or procaine benzylpenicillin into muscle.[3][10] During times of penicillin unavailability, ceftriaxone may be an alternative.[10] Where there is penicillin allergy, antimicrobial desensitisation is an option.[10][12]
Syphilis affects around one million pregnancies a year.[13] In 2016, there were around 473 cases of congenital syphilis per 100,000 live births and 204,000 deaths from the disease worldwide.[14] Of the 660,000 congenital syphilis cases reported in 2016, 143,000 resulted in deaths of unborn babies, 61,000 deaths of newborn babies, 41,000 low birth weights or preterm births, and 109,000 young children diagnosed with congenital syphilis.[15] Around 75% were from the WHO's African and Eastern Mediterranean regions.[2] Serological tests for syphilis were introduced in 1906, and it was later shown that transmission occurred from the mother.[16]
- ^ a b c Ghanem, Khalil G.; Hook, Edward W. (2020). "303. Syphilis". In Goldman, Lee; Schafer, Andrew I. (eds.). Goldman-Cecil Medicine. Vol. 2 (26th ed.). Philadelphia: Elsevier. p. 1986. ISBN 978-0-323-55087-1.
- ^ a b c d e f g Adamson, Paul C.; Klausner, Jeffrey D. (2022). "60. Syphilis (Treponema palladium)". In Jong, Elaine C.; Stevens, Dennis L. (eds.). Netter's Infectious Diseases (2nd ed.). Philadelphia: Elsevier. pp. 339–347. ISBN 978-0-323-71159-3.
- ^ a b c Ferri, Fred F. (2022). "Syphilis". Ferri's Clinical Advisor 2022. Philadelphia: Elsevier. pp. 1452–1454. ISBN 978-0-323-75571-9.
- ^ a b c d e f g h i j k l m n o p q r s Medoro, Alexandra K.; Sánchez, Pablo J. (June 2021). "Syphilis in Neonates and Infants". Clinics in Perinatology. 48 (2): 293–309. doi:10.1016/j.clp.2021.03.005. ISSN 1557-9840. PMID 34030815. S2CID 235200042. Archived from the original on 2022-07-20. Retrieved 2023-05-10.
- ^ a b James, William D.; Elston, Dirk; Treat, James R.; Rosenbach, Misha A.; Neuhaus, Isaac (2020). "18. Syphilis, Yaws, Bejel, and Pinta". Andrews' Diseases of the Skin: Clinical Dermatology (13th ed.). Edinburgh: Elsevier. pp. 347–361. ISBN 978-0-323-54753-6.
- ^ a b "STD Facts - Congenital Syphilis". www.cdc.gov. 10 April 2023. Archived from the original on 21 April 2023. Retrieved 9 May 2023.
- ^ Cite error: The named reference
Cooperwas invoked but never defined (see the help page). - ^ Gilmour, Leeyan S.; Walls, Tony (15 March 2023). "Congenital Syphilis: a Review of Global Epidemiology". Clinical Microbiology Reviews. 36 (2): e0012622. doi:10.1128/cmr.00126-22. ISSN 1098-6618. PMC 10283482. PMID 36920205. S2CID 257535283.
- ^ "Congenital Syphilis". Centers for Disease Control and Prevention. 1 April 2021. Archived from the original on 13 April 2023. Retrieved 12 May 2023.
- ^ a b c d e "Congenital Syphilis - STI Treatment Guidelines". www.cdc.gov. 19 October 2022. Archived from the original on 1 April 2023. Retrieved 9 May 2023.
- ^ WHO guideline on syphilis screening and treatment for pregnant women. Geneva: World health Organization. 2017. ISBN 978-92-4-155009-3.
- ^ Chastain, DB; Hutzley, VJ; Parekh, J; Alegro, JVG (9 August 2019). "Antimicrobial Desensitization: A Review of Published Protocols". Pharmacy. 7 (3): 112. doi:10.3390/pharmacy7030112. PMC 6789802. PMID 31405062.
- ^ Hussain, Syed A.; Vaidya, Ruben (2023). "Congenital Syphilis". StatPearls. StatPearls Publishing. PMID 30725772. Archived from the original on 2022-12-10. Retrieved 2023-05-12.
- ^ Global progress report on HIV, viral hepatitis and sexually transmitted infections, 2021 (PDF). Geneva: World Health Organization. 2021. ISBN 978-92-4-003098-5. Archived (PDF) from the original on 2023-03-26. Retrieved 2023-05-08.
- ^ "Congenital syphilis - Mother-to-child transmission of syphilis". www.who.int. Archived from the original on 21 April 2023. Retrieved 9 May 2023.
- ^ Oriel, J. David (2012). "5. "The sins of the fathers": Congenital syphilis". The Scars of Venus: A History of Venereology. London: Springer-Verlag. pp. 69–70. ISBN 978-1-4471-2068-1.