| Fecal incontinence | |
|---|---|
| Other names | Faecal incontinence, bowel incontinence, anal incontinence, accidental bowel leakage |
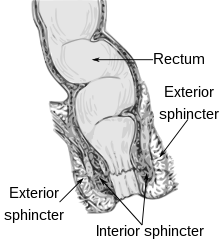 | |
| A diagram showing normal anatomy of the anal canal and rectum. | |
| Specialty | Gastroenterology |
| Causes | Puerperal disorder, ulcerative colitis |
| Medication | cholestyramine |
| Frequency | 2.2% |
Fecal incontinence (FI), or in some forms, encopresis, is a lack of control over defecation, leading to involuntary loss of bowel contents — including flatus (gas), liquid stool elements and mucus, or solid feces. FI is a sign or a symptom, not a diagnosis. Incontinence can result from different causes and might occur with either constipation or diarrhea. Continence is maintained by several interrelated factors, including the anal sampling mechanism, and incontinence usually results from a deficiency of multiple mechanisms. The most common causes are thought to be immediate or delayed damage from childbirth, complications from prior anorectal surgery (especially involving the anal sphincters or hemorrhoidal vascular cushions), altered bowel habits (e.g., caused by irritable bowel syndrome, Crohn's disease, ulcerative colitis, food intolerance, or constipation with overflow incontinence).[1] An estimated 2.2% of community-dwelling adults are affected.[2] However, reported prevalence figures vary. A prevalence of 8.39% among non-institutionalized U.S adults between 2005 and 2010 has been reported, and among institutionalized elders figures come close to 50%.[3][4]
Fecal incontinence has three main consequences: local reactions of the perianal skin and urinary tract, including maceration (softening and whitening of the skin due to continuous moisture), urinary tract infections, or decubitus ulcers (pressure sores);[1] a financial expense for individuals (due to the cost of medication and incontinence products, and loss of productivity), employers (days off), and medical insurers and society generally (health care costs, unemployment);[1] and an associated decrease in quality of life.[5] There is often reduced self-esteem, shame, humiliation, depression, a need to organize life around easy access to a toilet, and avoidance of enjoyable activities.[1] FI is an example of a stigmatized medical condition, which creates barriers to successful management and makes the problem worse.[6] People may be too embarrassed to seek medical help and attempt to self-manage the symptom in secrecy from others.
FI is one of the most psychologically and socially debilitating conditions in an otherwise healthy individual and is generally treatable.[2] More than 50% of hospitalized seriously ill patients rated bladder or fecal incontinence as "worse than death".[7] Management may be achieved through an individualized mix of dietary, pharmacologic, and surgical measures. Health care professionals are often poorly informed about treatment options,[2] and may fail to recognize the effect of FI.[5]
- ^ a b c d Cite error: The named reference
ASCRS core subjects FIwas invoked but never defined (see the help page). - ^ a b c Cite error: The named reference
ASCRS textbookwas invoked but never defined (see the help page). - ^ Ditah I, Devaki P, Luma HN, Ditah C, Njei B, Jaiyeoba C, et al. (April 2014). "Prevalence, trends, and risk factors for fecal incontinence in United States adults, 2005-2010". Clinical Gastroenterology and Hepatology. 12 (4): 636–643.e1–2. doi:10.1016/j.cgh.2013.07.020. PMID 23906873.
- ^ Nelson R, Furner S, Jesudason V (October 1998). "Fecal incontinence in Wisconsin nursing homes: prevalence and associations". Diseases of the Colon and Rectum. 41 (10): 1226–1229. doi:10.1007/bf02258218. PMID 9788384. S2CID 25800286.
- ^ a b Cite error: The named reference
Yamada textbookwas invoked but never defined (see the help page). - ^ "My bladder and bowel own my life." A collaborative workshop addressing the need for continence research (PDF). Age UK. 2018.
- ^ Rubin EB, Buehler AE, Halpern SD (October 2016). "States Worse Than Death Among Hospitalized Patients With Serious Illnesses". JAMA Internal Medicine. 176 (10): 1557–1559. doi:10.1001/jamainternmed.2016.4362. PMC 6848972. PMID 27479808.