| Nosebleed | |
|---|---|
| Other names | Epistaxis, bloody nose, nasal hemorrhage[1] |
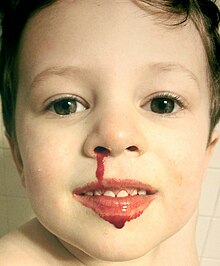 | |
| A three-year-old child with a minor nosebleed from falling and hitting his face on the floor | |
| Pronunciation |
|
| Specialty | Otorhinolaryngology |
| Symptoms | Bleeding from the nose[1] |
| Usual onset | Less than 10 and over 50 years old[2] |
| Risk factors | Trauma, excessive nose picking, certain infections, blood thinners, high blood pressure, alcoholism, seasonal allergies, dry weather[3] |
| Diagnostic method | Direct observation[1] |
| Differential diagnosis | Bleeding from the lungs, esophageal varices,[1] vomiting blood |
| Prevention | Petroleum jelly in the nose[4] |
| Treatment | Pressure over the lower half of the nose, nasal packing, endoscopy[5] |
| Medication | Tranexamic acid[6] |
| Frequency | 60% at some point in time[7] |
| Deaths | Rare[3] |
A nosebleed, also known as epistaxis, is an instance of bleeding from the nose.[1] Blood can flow down into the stomach, and cause nausea and vomiting.[8] In more severe cases, blood may come out of both nostrils.[9] Rarely, bleeding may be so significant that low blood pressure occurs.[1] Blood may also be forced to flow up and through the nasolacrimal duct and out of the eye, producing bloody tears.[10]
Risk factors include trauma, including putting the finger in the nose, blood thinners, high blood pressure, alcoholism, seasonal allergies, dry weather, and inhaled corticosteroids.[3] There are two types: anterior, which is more common; and posterior, which is less common but more serious.[3] Anterior nosebleeds generally occur from Kiesselbach's plexus while posterior bleeds generally occur from the sphenopalatine artery or Woodruff's plexus.[3] The diagnosis is by direct observation.[1]
Prevention may include the use of petroleum jelly in the nose.[4] Initially, treatment is generally the application of pressure for at least five minutes over the lower half of the nose.[5] If this is not sufficient, nasal packing may be used.[5] Tranexamic acid may also be helpful.[6] If bleeding episodes continue, endoscopy is recommended.[5]
About 60% of people have a nosebleed at some point in their life.[7] About 10% of nosebleeds are serious.[7] Nosebleeds are rarely fatal, accounting for only 4 of the 2.4 million deaths in the U.S. in 1999.[11] Nosebleeds most commonly affect those younger than 10 and older than 50.[2]
- ^ a b c d e f g Ferri, Fred F. (2013). Ferri's Clinical Advisor 2014 E-Book: 5 Books in 1. Elsevier Health Sciences. p. 399. ISBN 978-0-323-08431-4.
- ^ a b Kucik, Corry J.; Clenney, Timothy (2005-01-15). "Management of epistaxis". American Family Physician. 71 (2): 305–311. ISSN 0002-838X. PMID 15686301.
- ^ a b c d e Tabassom, A; Cho, JJ (January 2020). "Epistaxis (Nose Bleed)". StatPearls. PMID 28613768.
- ^ a b Morgan, Daniel J.; Kellerman, Rick (March 2014). "Epistaxis". Primary Care: Clinics in Office Practice. 41 (1): 63–73. doi:10.1016/j.pop.2013.10.007. ISSN 0095-4543. PMID 24439881.
- ^ a b c d Tunkel, David E.; Anne, Samantha; Payne, Spencer C.; Ishman, Stacey L.; Rosenfeld, Richard M.; Abramson, Peter J.; Alikhaani, Jacqueline D.; Benoit, Margo McKenna; Bercovitz, Rachel S.; Brown, Michael D.; Chernobilsky, Boris; Feldstein, David A.; Hackell, Jesse M.; Holbrook, Eric H.; Holdsworth, Sarah M.; Lin, Kenneth W.; Lind, Meredith Merz; Poetker, David M.; Riley, Charles A.; Schneider, John S.; Seidman, Michael D.; Vadlamudi, Venu; Valdez, Tulio A.; Nnacheta, Lorraine C.; Monjur, Taskin M. (7 January 2020). "Clinical Practice Guideline: Nosebleed (Epistaxis) Executive Summary". Otolaryngology–Head and Neck Surgery. 162 (1): 8–25. doi:10.1177/0194599819889955. PMID 31910122. S2CID 210072386.
- ^ a b Joseph, Jonathan; Martinez-Devesa, Pablo; Bellorini, Jenny; Burton, Martin J (2018-12-31). Cochrane ENT Group (ed.). "Tranexamic acid for patients with nasal haemorrhage (epistaxis)". Cochrane Database of Systematic Reviews. 2018 (12): CD004328. doi:10.1002/14651858.CD004328.pub3. PMC 6517002. PMID 30596479.
- ^ a b c Wackym, James B. Snow,... P. Ashley (2009). Ballenger's otorhinolaryngology : head and neck surgery (17th ed.). Shelton, Conn.: People's Medical Pub. House/B C Decker. p. 551. ISBN 9781550093377.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ Wilson, I. Dodd (1990). Walker, H. Kenneth; Hall, W. Dallas; Hurst, J. Willis (eds.). Clinical Methods: The History, Physical, and Laboratory Examinations (3rd ed.). Boston: Butterworths. ISBN 978-0409900774. PMID 21250251.
- ^ Krulewitz, NA; Fix, ML (February 2019). "Epistaxis". Emergency Medicine Clinics of North America. 37 (1): 29–39. doi:10.1016/j.emc.2018.09.005. PMID 30454778. S2CID 242676103.
- ^ Riordan-Eva, Paul (2000). Vaughan and Asbury's General Ophthalmology. McGraw Hill Professional. p. 92. ISBN 978-0-07-137831-4.
- ^ "Work Table I. Deaths from each cause by 5-year age groups, race and sex: US, 1999" (PDF). CDC. 2011. p. 1922. Retrieved 13 April 2020.