This article needs additional citations for verification. (September 2024) |
| Paratyphoid fever | |
|---|---|
| Other names | Paratyphoid |
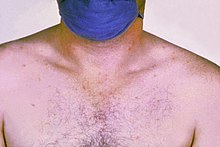 | |
| Rose colored spots on the chest of a man with typhoid fever, similar to those of paratyphoid | |
| Specialty | Infectious disease |
| Symptoms | Fever, headache, rash, weakness[1][2] |
| Usual onset | 6–30 days post-exposure[1][3] |
| Duration | Weeks to months[1] |
| Causes | Salmonella enterica spread by food or water contaminated with feces[1] |
| Risk factors | Poor sanitation, crowded populations[4] |
| Diagnostic method | Culturing the bacteria or detecting its DNA in the blood, stool, or bone marrow[1][3] |
| Prevention | Handwashing, clean water[1] |
| Treatment | Antibiotics[1] |
| Frequency | 529,000[5] |
| Deaths | 29,200[6] |
Paratyphoid fever, also known simply as paratyphoid, is a bacterial infection caused by one of three types of Salmonella enterica.[1] Symptoms usually begin 6–30 days after exposure and are the same as those of typhoid fever.[1][3] Often, a gradual onset of a high fever occurs over several days.[1] Weakness, loss of appetite, and headaches also commonly occur.[1] Some people develop a skin rash with rose-colored spots.[2] Without treatment, symptoms may last weeks or months.[1] Other people may carry the bacteria without being affected; however, they are still able to spread the disease to others.[3] Typhoid and paratyphoid are of similar severity.[3] Paratyphoid and typhoid fever are types of enteric fever.[7]
Paratyphoid is caused by the bacterium Salmonella enterica of the serotypes Paratyphi A, Paratyphi B, or Paratyphi C growing in the intestines and blood.[1] They are usually spread by eating or drinking food or water contaminated with the feces of an infected person.[1] They may occur when a person who prepares food is infected.[2] Risk factors include poor sanitation as is found among poor crowded populations.[4] Occasionally, they may be transmitted by sex.[1] Humans are the only animals infected.[1] Diagnosis may be based on symptoms and confirmed by either culturing the bacteria or detecting the bacterial DNA in the blood, stool, or bone marrow.[1][3] Culturing the bacteria can be difficult.[3] Bone-marrow testing is the most accurate.[4] Symptoms are similar to those of many other infectious diseases.[3] Typhus is a different disease.[8]
While no vaccine is available specifically for paratyphoid, the typhoid vaccine may provide some benefit.[1][2] Prevention includes drinking clean water, better sanitation, and better handwashing.[1] Treatment of the disease is with antibiotics such as azithromycin.[1] Resistance to a number of other previously effective antibiotics is common.[1]
Paratyphoid affects about six million people a year.[1][9] It is most common in parts of Asia and rare in the developed world.[1][2] Most cases are due to Paratyphi A rather than Paratyphi B or C.[3] In 2015, paratyphoid fever resulted in about 29,200 deaths, down from 63,000 deaths in 1990.[10][6] The risk of death is between 10% and 15% without treatment, while with treatment, it may be less than 1%.[3]
- ^ a b c d e f g h i j k l m n o p q r s t u v w Newton, Anna E. (2014). "3 Infectious Diseases Related To Travel". CDC health information for international travel 2014: the yellow book. Oup USA. ISBN 9780199948499. Archived from the original on 2 July 2015.
- ^ a b c d e Hawker, Jeremy (2012). "3.56". Communicable disease control and health protection handbook (3rd ed.). Chichester, UK: Wiley-Blackwell. ISBN 9781444346947. Archived from the original on 8 September 2017.
- ^ a b c d e f g h i j Magill, Alan J. (2013). Hunter's tropical medicine and emerging infectious diseases (9th ed.). London: Saunders/Elsevier. pp. 568–572. ISBN 9781455740437. Archived from the original on 8 September 2017.
- ^ a b c Crump, JA; Mintz, ED (15 January 2010). "Global trends in typhoid and paratyphoid Fever". Clinical Infectious Diseases. 50 (2): 241–246. doi:10.1086/649541. PMC 2798017. PMID 20014951.
- ^ GBD 2015 Disease and Injury Incidence and Prevalence Collaborators (8 October 2016). "Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015". The Lancet. 388 (10053): 1545–1602. doi:10.1016/S0140-6736(16)31678-6. PMC 5055577. PMID 27733282.
- ^ a b GBD 2015 Mortality and Causes of Death Collaborators (8 October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015". The Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ^ Wain, J; Hendriksen, RS; Mikoleit, ML; Keddy, KH; Ochiai, RL (21 March 2015). "Typhoid fever". The Lancet. 385 (9973): 1136–1145. doi:10.1016/s0140-6736(13)62708-7. PMC 11567078. PMID 25458731. S2CID 1499916.
- ^ Cunha, BA (March 2004). "Osler on typhoid fever: differentiating typhoid from typhus and malaria". Infect. Dis. Clin. North Am. 18 (1): 111–125. doi:10.1016/S0891-5520(03)00094-1. PMID 15081508.
- ^ Global Burden of Disease Study 2013 Collaborators (22 August 2015). "Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013". The Lancet. 386 (9995): 743–800. doi:10.1016/s0140-6736(15)60692-4. PMC 4561509. PMID 26063472.
- ^ GBD 2013 Mortality and Causes of Death Collaborators (17 December 2014). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013". The Lancet. 385 (9963): 117–71. doi:10.1016/S0140-6736(14)61682-2. PMC 4340604. PMID 25530442.