| Status epilepticus | |
|---|---|
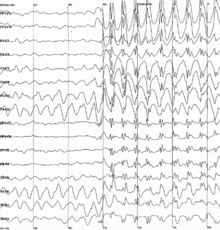 | |
| Generalized 3 Hz spike-and-wave discharges on an electroencephalogram | |
| Specialty | Emergency medicine, neurology |
| Symptoms | Regular pattern of contraction and extension of the arms and legs, movement of one part of the body, unresponsive[1] |
| Duration | >5 minutes[1] |
| Risk factors | Epilepsy, underlying problem with the brain[2] |
| Diagnostic method | Blood sugar, imaging of the head, blood tests, electroencephalogram[1] |
| Differential diagnosis | Psychogenic nonepileptic seizures, movement disorders, meningitis, delirium[1] |
| Treatment | Benzodiazepines, fosphenytoin, phenytoin,[1] paraldehyde (rarely used) |
| Prognosis | ~20% thirty-day risk of death[1] |
| Frequency | 40 per 100,000 people per year[2] |
Status epilepticus (SE), or status seizure, is a medical condition consisting of a single seizure lasting more than 5 minutes, or 2 or more seizures within a 5-minute period without the person returning to normal between them.[3][1] Previous definitions used a 30-minute time limit.[2] The seizures can be of the tonic–clonic type, with a regular pattern of contraction and extension of the arms and legs, or of types that do not involve contractions, such as absence seizures or complex partial seizures.[1] Status epilepticus is a life-threatening medical emergency, particularly if treatment is delayed.[1]
Status epilepticus may occur in those with a history of epilepsy as well as those with an underlying problem of the brain.[2] These underlying brain problems may include trauma, infections, or strokes, among others.[2][4] Diagnosis often involves checking the blood sugar, imaging of the head, a number of blood tests, and an electroencephalogram.[1] Psychogenic nonepileptic seizures may present similarly to status epilepticus.[1] Other conditions that may also appear to be status epilepticus include low blood sugar, movement disorders, meningitis, and delirium, among others.[1] Status epilepticus can also appear when tuberculous meningitis becomes very severe.
Benzodiazepines are the preferred initial treatment, after which typically phenytoin is given.[1] Possible benzodiazepines include intravenous lorazepam as well as intramuscular injections of midazolam.[5] A number of other medications may be used if these are not effective, such as phenobarbital, propofol, or ketamine.[1] After initial treatment with benzodiazepines, typical antiseizure drugs should be given, including valproic acid (valproate), fosphenytoin, levetiracetam, or a similar substance(s).[6] While empirically based treatments exist, few head-to-head clinical trials exist, so the best approach remains undetermined.[6] This said, "consensus-based" best practices are offered by the Neurocritical Care Society.[6] Intubation may be required to help maintain the person's airway.[1] Between 10% and 30% of people who have status epilepticus die within 30 days.[1] The underlying cause, the person's age, and the length of the seizure are important factors in the outcome.[2] Status epilepticus occurs in up to 40 per 100,000 people per year.[2] Those with status epilepticus make up about 1% of people who visit the emergency department.[1]
- ^ a b c d e f g h i j k l m n o p q Al-Mufti, F; Claassen, J (Oct 2014). "Neurocritical Care: Status Epilepticus Review". Critical Care Clinics. 30 (4): 751–764. doi:10.1016/j.ccc.2014.06.006. PMID 25257739.
- ^ a b c d e f g Trinka, E; Höfler, J; Zerbs, A (September 2012). "Causes of status epilepticus". Epilepsia. 53 (Suppl 4): 127–38. doi:10.1111/j.1528-1167.2012.03622.x. PMID 22946730. S2CID 5294771.
- ^ Drislane, Frank (19 March 2020). Garcia, Paul; Edlow, Jonathan (eds.). "Convulsive status epilepticus in adults: Classification, clinical features, and diagnosis". UpToDate. 34.2217. Wolters Kluwer.
- ^ Trinka, E., Cock, H., Hesdorffer, D., Rossetti, A. O., Scheffer, I. E., Shinnar, S., Shorvon, S., & Lowenstein, D. H. (2015). A definition and classification of status epilepticus--Report of the ILAE Task Force on Classification of Status Epilepticus. Epilepsia, 56(10), 1515–1523. doi:10.1111/epi.13121
- ^ Prasad, M; Krishnan, PR; Sequeira, R; Al-Roomi, K (Sep 10, 2014). "Anticonvulsant therapy for status epilepticus". The Cochrane Database of Systematic Reviews. 2014 (9): CD003723. doi:10.1002/14651858.CD003723.pub3. PMC 7154380. PMID 25207925.
- ^ a b c Drislane, Frank (15 June 2021). Garcia, Paul; Edlow, Jonathan (eds.). "Convulsive status epilepticus in adults: Treatment and prognosis: Initial Treatment". UpToDate. 52.96933. Wolters Kluwer.