| Vasectomy | |
|---|---|
 | |
| Background | |
| Type | Sterilization |
| First use | 1899 (experiments from 1785)[1] |
| Failure rates (first year) | |
| Perfect use | 0.10%[2] |
| Typical use | 0.15%[2] "Vas-Clip" nearly 1% |
| Usage | |
| Duration effect | Permanent |
| Reversibility | Possible |
| User reminders | A negative semen specimen is required to verify no sperm.[3] |
| Clinic review | All |
| Advantages and disadvantages | |
| STI protection | No |
| Benefits | No need for general anesthesia. Lower cost and less invasive than tubal ligation for females. |
| Risks | Temporary local inflammation of the testes, long-term genital pain. |
This section needs additional citations for verification. (March 2024) |
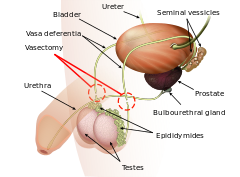
Vasectomy is an elective surgical procedure that results in male sterilization, often as a means of permanent contraception. During the procedure, the male vasa deferentia are cut and tied or sealed so as to prevent sperm from entering into the urethra and thereby prevent fertilization of a female through sexual intercourse. Vasectomies are usually performed in a physician's office, medical clinic, or, when performed on a non-human animal, in a veterinary clinic. Hospitalization is not normally required as the procedure is not complicated, the incisions are small, and the necessary equipment routine.
There are several methods by which a surgeon might complete a vasectomy procedure, all of which occlude (i.e., "seal") at least one side of each vas deferens. To help reduce anxiety and increase patient comfort, those who have an aversion to needles may consider a "no-needle" application of anesthesia while the 'no-scalpel' or 'open-ended' techniques help to accelerate recovery times and increase the chance of healthy recovery.[4]
Due to the simplicity of the surgery, a vasectomy usually takes less than 30 minutes to complete. After a short recovery at the doctor's office (usually less than an hour), the patient is sent home to rest. Because the procedure is minimally invasive, many vasectomy patients find that they can resume their typical sexual behavior within a week, and do so with little or no discomfort.
Because the procedure is considered a permanent method of contraception and is not easily reversed, patients are frequently counseled and advised to consider how the long-term outcome of a vasectomy might affect them both emotionally and physically. The procedure is not typically encouraged for young single childless people as their risk of later regret is higher as chances of biological parenthood are thereby permanently reduced, often completely.[citation needed] A vasectomy without the patient's consent or knowledge is considered forced sterilization.
- ^ Cite error: The named reference
popenoewas invoked but never defined (see the help page). - ^ a b Trussell J (2011). "Contraceptive efficacy". In Hatcher RA, Trussell J, Nelson AL, Cates W Jr, Kowal D, Policar MS (eds.). Contraceptive technology (20th revised ed.). New York: Ardent Media. pp. 779–863. ISBN 978-1-59708-004-0. ISSN 0091-9721. OCLC 781956734. Table 26–1 = Table 3–2 Percentage of women experiencing an unintended pregnancy during the first year of typical use and the first year of perfect use of contraception, and the percentage continuing use at the end of the first year. United States.
- ^ "Information for Patients - Vasectomy Semen Analysis" (PDF). Manchester University NHS Foundation Trust. May 2017. Retrieved 13 March 2023.
- ^ "What Happens When I Get a Vasectomy?". WebMD. Retrieved 7 October 2021.